
How To Get a Portable Oxygen Concentrator Covered By Medicare
A portable oxygen concentrator is a medical device that purifies the air you breathe. These devices are substantially smaller than oxygen tanks, allowing persons who use oxygen to maintain their mobility and lifestyle choices. Is a portable oxygen concentrator covered by Medicare?
Related Topics (Sponsored Ads):
While Original Medicare covers oxygen and oxygen tanks (typically in the form of equipment rentals), it does not cover personal oxygen concentrators (POCs) due to their high cost. Instead than buying oxygen tanks, Medicare can usually save money by renting them. While most Medicare Advantage plans provide more benefits above Original Medicare, POCs may be excluded for the same reason. Whether you’re interested in a POC, check with your insurance provider to see if it’s covered.
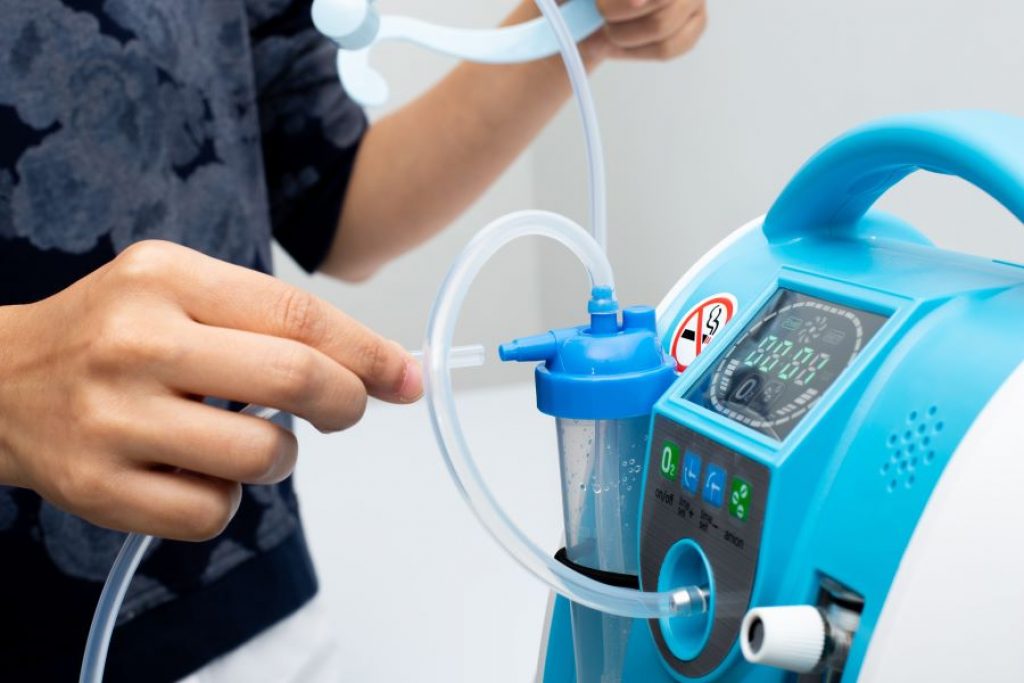
Why Do Oxygen Concentrators Cost So Much?
Because portable oxygen concentrators are intricate pieces of technology, they are costly. They feature internal mechanisms that allow them to take ordinary air from wherever you are and turn it mostly into oxygen. They may also run on battery power, which necessitates a high level of efficiency.
Is an Oxygen Tank or an Oxygen Concentrator Better?
Portable oxygen concentrators may be expensive, and patients often have to pay for them out of pocket since Medicare does not cover them. POCs must also be fueled by a battery or an electrical outlet, so you should plan on utilizing one to get the most out of features like flexibility and mobility. Medicare covers oxygen tanks, lowering your out-of-pocket costs significantly (at least up front). However, they are less adaptable and might limit your movement. In the end, you’ll have to consider your particular demands as well as your budget to choose which choice is best for you.
The following is a must in order for Medicare to fund oxygen equipment:
You must have a doctor’s prescription.
Have proof from your doctor that you have a lung problem that prevents you from getting adequate oxygen and that prior treatments have failed to improve your condition.
Your doctor must provide proof of gas levels in your blood.
Renting oxygen equipment from a participating DME provider is more cost-effective. Your rent will be paid for up to three years. After then, the equipment will remain in the supplier’s possession. They must, however, continue to provide oxygen to you for another 24 months. If you still need oxygen treatment after 5 years, you have the option of renewing your contract with your current provider or finding a new one.
What Does It Cost to Get Oxygen on Medicare?
Canned oxygen at a concentration of roughly 95% typically costs around $50 per unit. If you depend on an oxygen machine all of the time, canned oxygen might be expensive. The price tag may swiftly rise to more than $1,160 per day and $426,000 per year!
You will only be liable for the 20% coinsurance if you have Part B coverage. Unfortunately, for most recipients, this is still too much to pay out of pocket. This is why many people choose for a Medicare Supplement plan to cover their coinsurance as well as other out-of-pocket expenses like deductibles.
Will Oxygen Therapy Be Covered by Medicare Advantage?
Medicare-approved health services and equipment must be covered by Advantage plans. Fortunately, oxygen is included in this group. However, since these plans are provided by private insurance firms, the price of coverage may vary.
The easiest way to find out whether oxygen treatment is covered is to call the insurance company. The carrier determines how much coverage they provide. As a result, they may cover it, but only to a lesser extent than Medicare would.
Related Topics (Sponsored Ads):
Discover More






